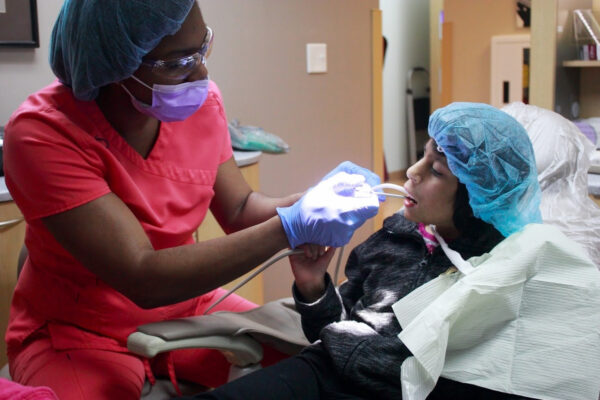
Dental Clinic
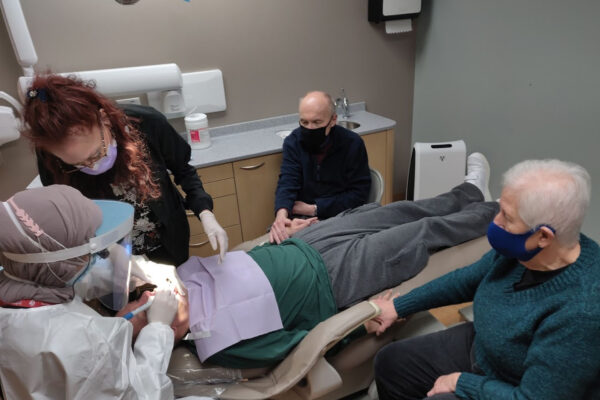
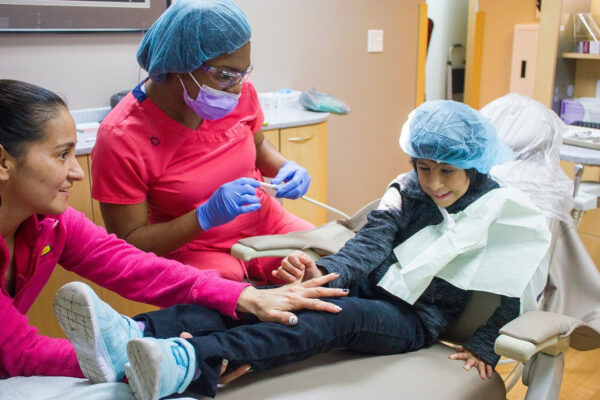
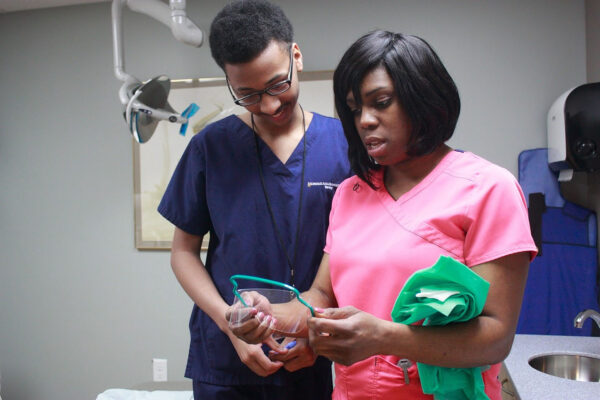
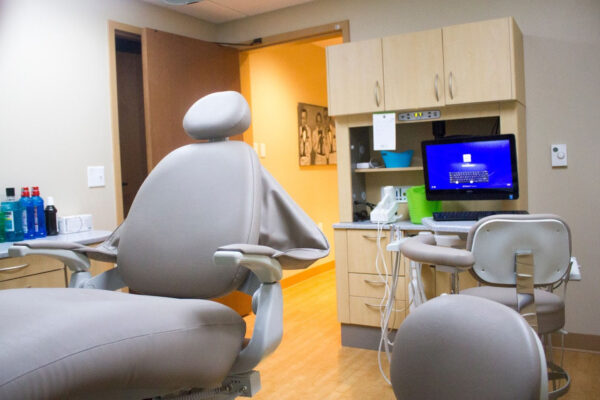
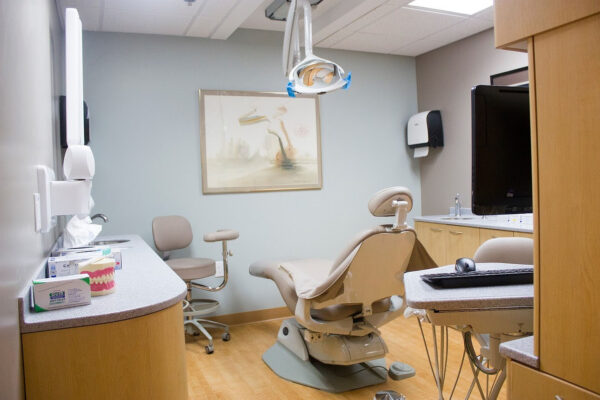
Located at the Bucyrus Campus, this unique dental clinic specifically serves children and adults with moderate to severe cognitive or physical disabilities that keep them from being treated in standard private practice or community clinics. Our dentists and hygienists are trained to treat clients with special needs, in a setting designed with features to make their care as comfortable as possible. Treatment rooms and hallways easily accommodate wheelchairs and scooters.
Patients are seen by appointment and need a referral from a dentist or medical doctor. They must be a Wisconsin resident.
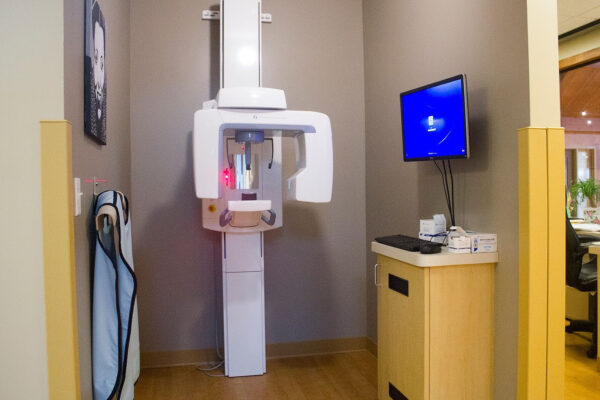
- Our Clinic provides dental exams and cleaning, fluoride treatments, and sealants. We also offer all forms of X-rays, endodontic and periodontal work, as well as restorative work (including fillings, crowns, and extractions).
- For an appointment or more information, call (414) 210-2440. The clinic is open 8 a.m. to 5 p.m., Monday, Tuesday, Thursday and Friday.
- We accept all forms of Medicaid. Other accepted insurances include United Healthcare, Humana, Envolve, Blue Cross Blue Shield, Dental Network of America, and Dental Professionals of Wisconsin.


Before Visiting Our Dental Clinic
Please contact the office to receive the Welcome Packet registration forms. Complete all forms and mail or drop them off to the clinic before your first visit.
Mail to:
Gardetto Family Community Dental Clinic
2450 W. North Ave.,
Milwaukee WI 53205.
Dental Clinic FAQs
Can anyone be seen at your Dental Clinic?
The Gardetto Family Community clinic is reserved specifically for Wisconsin children and adults with moderate to severe cognitive or physical disabilities that prevent them from being treated in standard private practice or community clinics. Prospective patients must have a referral from a doctor or dentist.
Do you take insurance?
We accept all forms of Medicaid. Other accepted insurances include United Healthcare, Humana, Envolve, Blue Cross Blue Shield, Dental Network of America, and Dental Professionals of Wisconsin.
The Gardetto Family Community Dental Clinic is supported in part by grants from the Delta Dental of Wisconsin Foundation, The Catholic Community Foundation, and the Green Bay Packers Foundation.
Let’s Connect
Our staff would love to hear from you! Submit your questions or feedback about our services, or inquiries about getting involved with St. Ann Center’s mission through the contact form below.
- Bucyrus Campus: (414) 210-2440
"*" indicates required fields